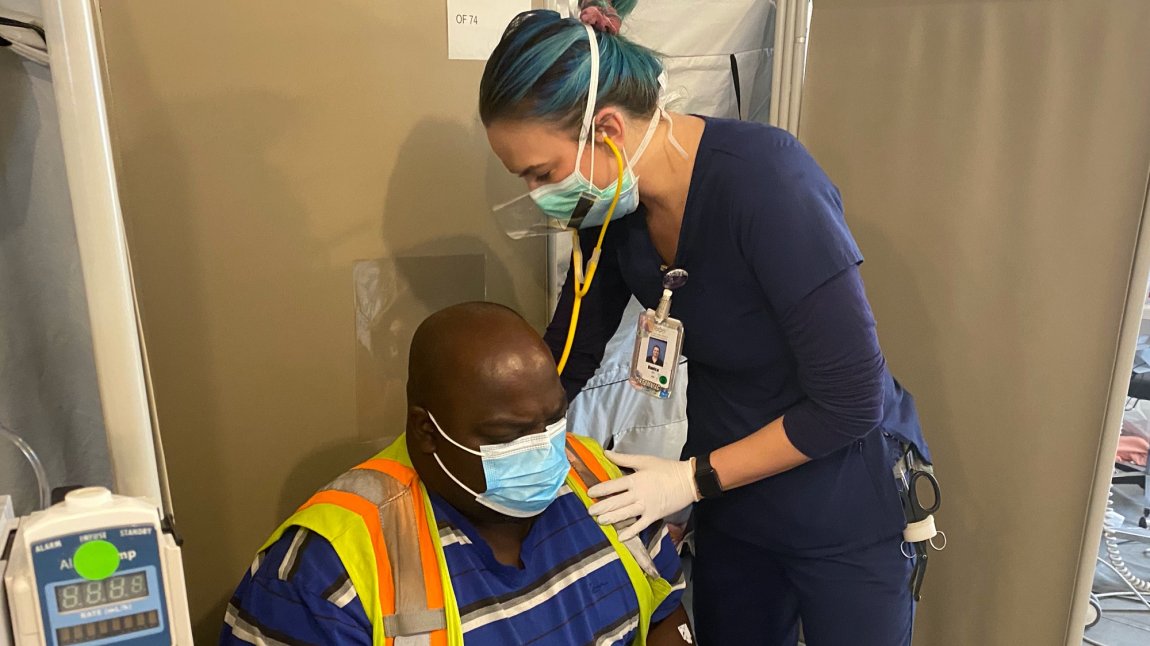
Inside a military-style MASH tent, a nurse with aqua blue hair and a mask across her face touches the arm of her patient, sitting heavily upon a folding chair.
This is Danica Riedlinger, at the very front lines in the fight against COVID-19, putting her life on the line for a cause and community she believes in.
“I feel like it’s part of who I am to step up and do my part for the community,” said Danica, 32, an Emergency Department nurse at the Martin Luther King, Jr. Community Hospital (MLKCH). “Part of why I became a nurse is to be involved in caring for people during events like this.”
Events like these—but there haven’t been events like this. Not this big. Not this complex.
It makes what Danica is doing—and hundreds of other front-line MLKCH staff—even more extraordinary. Hundreds of doctors and nurses in the United States have been sickened, some critically, by the virus. Supplies of basic protective equipment—masks, gloves, robes—are in short supply across California and the nation.
MLKCH staff know they are putting their lives on the line. And they are still here.